When my son Matthew was born with severe Hemophilia A in 1994, I thought I was prepared. I had been raised by a Dad with hemophilia, lost him to HIV in 1986, and had thoroughly researched product safety prior to deciding to give birth to my son. I had prenatal testing done and knew that I was expecting a baby with hemophilia. My husband and I interviewed several hematologists who assured us that clotting factor therapy was safe and effective, and that a child born with hemophilia in the United States in 1994 could expect to live a pretty normal life. We even attended some Hemophilia Treatment Center (HTC) events, and visited with other young hemophilia families. Encouraged, we settled in and looked forward to having our second child.
Matthew was born normally, with no complications. He experienced no bleeds and required no treatment until he had an elective surgery to correct a foot defect when he was six months old. During that surgery he had a central venous access line placed, and received his first doses of recombinant clotting factor. The idea was that he would begin prophylaxis to have less bleeding episodes. Within a week he developed a high titer inhibitor.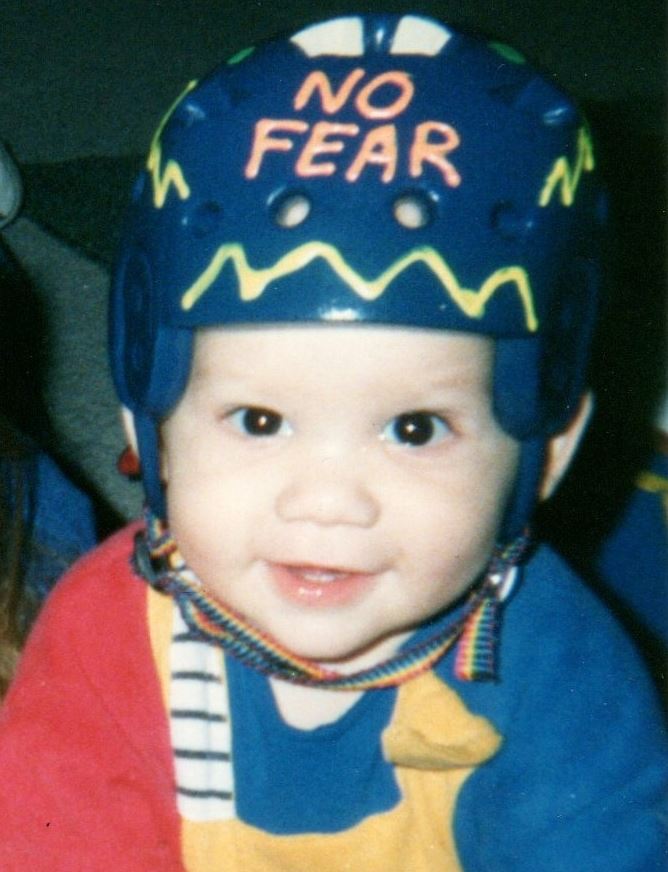 We had been told nothing about inhibitors in all our previous talks with hematologists, HTC staff, and other families. Growing up in the hemophilia community, I had never met another person with an inhibitor. My father had always responded well to clotting factors and had even had several major surgeries that were successfully managed with plasma derived clotting factors (until he contracted HIV in 1982). So to say the least, I was very upset and unprepared for my son’s diagnosis of an inhibitor.
We had been told nothing about inhibitors in all our previous talks with hematologists, HTC staff, and other families. Growing up in the hemophilia community, I had never met another person with an inhibitor. My father had always responded well to clotting factors and had even had several major surgeries that were successfully managed with plasma derived clotting factors (until he contracted HIV in 1982). So to say the least, I was very upset and unprepared for my son’s diagnosis of an inhibitor.
I had my son’s genetic mutation analyzed and it turned out that my family’s hemophilia gene mutation is not known to be at risk for inhibitors. We tried everything recommended by my son’s physicians to eradicate his inhibitor. We began Immune Tolerance Therapy (ITT) right away when his inhibitor titer was at its lowest. We used a high dose protocol. We switched to a plasma-derived product that contained von Willebrand Factor (vWD). We added immune suppressants and IVIG. We even tried a risky procedure called plasmapheresis to try to remove the circulating antibodies. Nothing was helping. My son’s inhibitor titer would fall a little bit and then just start climbing back up again.
We used the best-known treatments to manage his bleeds. He got approved to use Novo Seven before it was even licensed in the United States. He was one of the first patients to ever use FEIBA and Novoseven prophylactically. He had care from some of the best hematologists and inhibitor experts in the world. Several researchers were interested and tried to help.
We tried to remain optimistic, but things just kept getting worse:
- Matt had infections from the central lines.
- We lost our health insurance (several times) because of the high costs of his treatment.
- He suffered bleed after bleed.
- We spent weeks and months in hospitals.
- He became physically addicted to pain medications.
- He ended up in a wheelchair most of the time and missed school more often then he went.
- I had to give up my career and stay home to care for him.
During this time I grew angrier and angrier that no one had warned me that this could happen. Â In 2002, something went terribly wrong. Matthew started complaining about headaches. We took him to see several doctors. They told us he had a cold or a virus. Doctors tested his blood, everything looked fine. They suggested he take more pain meds. But the headaches kept getting worse.
Suddenly one day, he couldn’t even sit up without crying in pain. Back to the HTC we went. This time he saw a different hematologist, someone who was in training. This doctor took a look at him, noticed his central line and said, “I think he might have a blood clot.” I am thinking, “No way, how stupid is this doctor, doesn’t he know that Matt has severe hemophilia and an inhibitor, his blood does NOT clot.”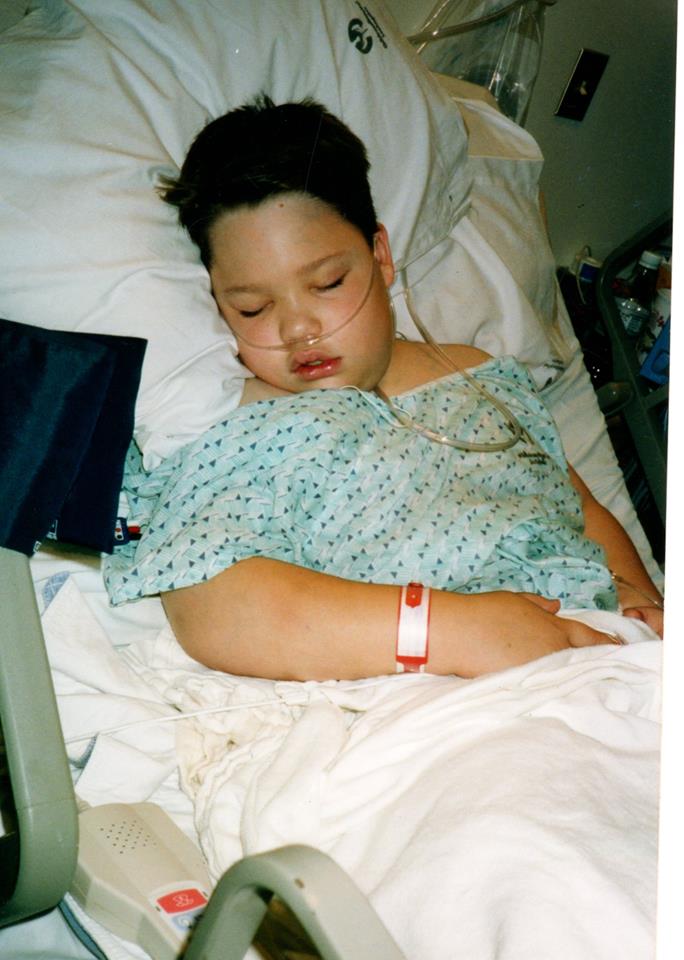
Off we went for an ultrasound and a dye study, and low and behold – yes – Matthew had a huge blood clot in his subclavian vein. It was above where his central line was threaded through the vein, so it wasn’t blocking the function of the catheter. But it was blocking almost all of the blood flow from his head back to his heart. More studies followed and they found that he had also had a huge old blood clot in his other subclavian vein where another central line had been 4 years earlier.
Matt was in big trouble. With both subclavian veins blocked, no blood was circulating from his upper body back through his heart. Things went downhill quickly. He spent the next three months in Intensive Care fighting for his life. His upper torso and head swelled up from all the backed up blood and fluid. He couldn’t breathe. He was in severe pain. He was so sick from all the pain meds and everything they were trying to do to clear the clots that he couldn’t eat – he vomited daily and didn’t eat anything for an entire month.
They put him on blood thinners. He developed a retroperitoneal bleed that got so bad it blocked the urine flow out of his kidneys. They didn’t want to treat the bleed because it might make the blood clots worse. He blew out one kidney, then the other. He started peeing buckets of blood. He had to have blood transfusions daily. Things just kept spiraling out of control.
Our family felt as if we were being ripped apart, both physically and emotionally. We were terrified. One day Matt’s vital signs crashed and they had to call a code blue. I wasn’t there that day, but the priest was called in. They were able to resuscitate him. When my husband called and told me what had happened, I just fell apart. Why had all of this happened? We did everything right and we followed all of our doctor’s orders. We were meticulous with his care, we were good parents. Why, Why, Why????
Eventually Matt did recover from that crisis. The blood clots never cleared, but he grew enough new veins for his blood to circulate. To this day he still cannot lay flat or the blood backs up into his head. He never tolerized to clotting factor. He now is confined to a wheelchair due to the joint damage from repeated bleeding in his knees. He has had several major surgeries to stop bleeding in his joints and try to relieve him from pain.
We have tried to make the best of the situation. Life goes on. Matt graduated from high school with good grades, and he is now in college. He has a girlfriend, he drives a car, and he has a job. He has coped amazingly well. He is a very intelligent, funny, and talented young man. But I still ask myself almost every day, “Why did this have to happen?” and “Why do so many others keep forming inhibitors?”
For twenty years now, I have watched as more and more kids and even adults with hemophilia develop inhibitors. I see them going through the same struggles that we have. I cry and laugh with them, visit them in hospitals, try to help them financially when I can, share information, and generally just try to hold many of their hands. But nothing ever seems to get any better. We don’t have any new treatments for inhibitors. Physicians haven’t figured out anything to try to prevent an inhibitor, many of them don’t even warn their patients of the risks. The costs for the same old medications, which aren’t very effective, just keep getting higher and higher. Scientists and treatment providers debate endlessly in medical journals about which products might have lower inhibitor risks. Regulators do nothing. Everyone keeps calling for more and more “studies.” Drug companies deny that there is anything that can be done and just try to say it is the person’s immune system or their “genetics”. They keep telling us their products are “safe and effective”.
We don’t have any new treatments for inhibitors. Physicians haven’t figured out anything to try to prevent an inhibitor, many of them don’t even warn their patients of the risks. The costs for the same old medications, which aren’t very effective, just keep getting higher and higher. Scientists and treatment providers debate endlessly in medical journals about which products might have lower inhibitor risks. Regulators do nothing. Everyone keeps calling for more and more “studies.” Drug companies deny that there is anything that can be done and just try to say it is the person’s immune system or their “genetics”. They keep telling us their products are “safe and effective”.
Our hemophilia organizations barely even mention inhibitors. Very few conferences include anything for inhibitor patients or try to educate the community about these risks or what dealing with an inhibitor is actually like. If anything is offered, it is just a “segregated” conference where many if us feel like a bunch of lost causes that don’t even really belong with the rest of the hemophilia community.
The companies that manufacture the treatments for inhibitor patients and the homecare companies that supply our products make more and more money off of us. Yet most inhibitor families can barely hold onto their jobs or get health insurance. Many struggle with paying basic bills.
Was someone to blame for all of this? Or was it just something that was “meant to be?” Is it supposed to make us stronger or better people? Is it God’s will? Should we find a way to “stay positive” and make the best out of all of this?
I have struggled with these questions for years and honestly I can say I just don’t know what to think anymore…but one thing I know for sure is this didn’t happen because our family or my son did anything wrong. What I have decided is – We did not fail treatment…the treatments failed us. The physicians failed us, the scientists failed us, the regulators failed us, the drug companies failed us, and even our hemophilia organizations have failed us. They are failing a lot of other families too. 
The Centers for Disease Control and Prevention in the United States conducted a 6-year study on inhibitors and found some surprising results. They found that everyone with hemophilia is at risk for developing an inhibitor. They also found that many people were not being tested regularly and some people actually had inhibitors and didn’t even know it. Read the study in its entirety.Â
Isn’t it time to address this for the thousands of families that are already affected and for the thousands more that will come after us? This isn’t the first time our community has faced something like this. If we don’t do it, who will?
- Stand Up
- Speak Out
- Create Change
That is what we are trying to do, it is all we have left to do.
Debbie Porter lives in Southern California. She has been involved with the hemophilia community for over 50 years. He father had severe hemophilia and passed away from HIV in 1986. She is a carrier, and has a 20 year old son with severe hemophilia and an inhibitor. Her daughter has mild hemophilia. She is a Certified Public Accountant and has been trained as a Registered Nurse. She has served on the Board of Directors or her local hemophilia foundation and participated in subcommittees for NHF. She has severed on consumer advisory panels for several pharmaceuticals companies and specialty pharmacies. She and her son, Matthew, started Reduce Inhibitor Development (RID) in 2013 to raise awareness about the issues surrounding inhibitors to hemophilia treatment. The goal of the RID is raise awareness about inhibitors in hemophilia and to encourage research and the implementation of solutions.
Note: This story was originally posted on Reduce Inhibitor Development (RID)Â Facebook page. HFA has republished it with permission from Debbie Porter.Â




